Reversing Alzheimer's: The Forgotten Causes And Cures Big Pharma Buried
Authored by A Midwestern Doctor via The Forgotten Side of Medicine,
•Due to Alzheimer’s research focusing on a symptom of it (amyloid plaques), rather than its actual cause, Alzheimer’s has remained “incurable” for decades.
•Rather than being a single disease, Alzheimer’s has multiple different subtypes (e.g., those due to insulin resistance, nutritional deficiencies, inflammation, infections, or concussions), each of which requires a different treatments.
•Impaired blood circulation to the brain and lymphatic drainage from the brain are often the primary trigger which initiates the degenerative process seen in Alzheimer’s disease.
•Factors which impair this circulation (e.g., poor sleep) hence roughly double the risk of dementia, while treatments which improve this circulation frequently produce remarkable improvements for cognitive decline and dementia.
•DMSO, an effective treatment for brain injuries like strokes is well suited to address many of the root causes of dementia and reverse the degenerative state dying neurons get trapped in. Because of this, there are many reports of it reversing dementia and clinical trials in both humans and animals corroborating these improvements.
•This article will review the actual causes of dementias like Alzheimer’s and the forgotten therapies many have successful used to cure them.
Alzheimer’s dementia is one of the greatest medical challenged our country faces (e.g., places an incredible burden upon society (e.g., last year it was estimated to cost the United States 360 billion dollars). Yet, despite spending billions for research each year, cures remain elusive, something many believe results from the flawed belief eliminating the amyloid plaques associated with Alzheimer’s will fix it.
In turn, as I showed here:
-
Decades of amyloid therapies have never produced a beneficial therapy.
-
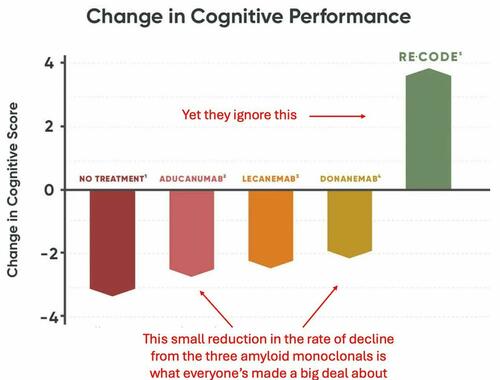
The newest “breakthrough” amyloid eliminating monoclonal antibodies, at best, slightly slow the progression of Alzheimer’s while simultaneously causing a host of side effective including brain bleeding and swelling in over a quarter of recipients.
-
The entire amyloid industry rests upon a fraudulent study no one wanted to retract, likely due to how much was invested in the amyloid hypothesis.
In short, the money behind this juggernaut has caused research into the real causes of Alzheimer’s to be suppressed. For example, here I highlighted how coconut oil MCT’s (safely) do more than any of the costly amyloid drugs—yet virtually no one knows this.
Dale Bredesen’s Discovery
Many are also unaware a 2022 study that should have revolutionized the entire Alzheimer’s field:
That protocol was based on the insightful realizations that:
• Amyloid protein is a protective mechanism the brain uses to protect itself from stressors that endanger brain tissue—making attempt to treat Alzheimer’s by eliminating it doomed to fail.
• The brain is designed to be able to adapt to the needs of life, so it is always creating or pruning neural connections and brain cells. Alzheimer’s results from the loss of signals that sustain brain cells and the dismantling of neural connections outweighing the formation of new ones gradually compounding over the decades.
• Rather than there being one type of Alzheimer’s, there are actually multiple that each require different treatment approaches.
Note: beyond the 2022 trial which showed individually targeted therapies could shift the brain’s momentum from neurological degeneration to regrowth, a 2018 report of 100 patients from numerous providers also showed it treated Alzheimer’s, as did a 2024 case series of patients with remarkable results, and there are now neurologists around the country administering Bredesen’s protocol with success.
The Six Types of Alzheimer’s Disease
As this understanding of Alzheimer’s has produced real results, this suggests the causes of Alzheimer’s Bredesen identified indeed play a key role in the disease—particularly since many other datasets corroborate their contribution to Alzheimer’s. They are as follows:
Type 1 — Inflammatory
This form is driven by excessive inflammation, often metabolic or infectious in nature. Chronic activation of the immune system—due to factors such as insulin resistance, a poor diet, a leaky gut, or latent infections—leads the brain to engage in protective downsizing by removing synapses and neurons that are less essential for immediate survival. It often presents with classic Alzheimer’s memory loss and typically develops in the sixties to seventies.
Type 1.5 — Glycotoxic
This subtype arises from insulin resistance and chronically elevated blood sugar. It leads to both inflammatory and trophic deficiencies, and is driven by glycotoxicity and the accumulation of advanced glycation end products (AGEs), which impair cellular function and synaptic integrity. It typically appears in the late fifties to sixties.
Note: chronically elevated insulin promotes amyloid formation as the enzyme the body uses to break down insulin is the same enzyme it uses to break down amyloid plaques.
Type 2 — Atrophic
This type is caused by deficiencies in key nutrients, hormones, and other factors that provide trophic (supportive) signals to brain cells which then triggers a similar downsizing mechanism seen in Type 1. Type 2 tends to emerge about a decade later than Type 1.
Note: we find these nutritional deficiencies can result from poor circulation reducing existing nutrients reaching brain tissue, and hence often focus on improving circulation rather than extended supplementation.
Type 3 — Toxic
This subtype results from exposure to toxic substances that directly damage neurons. Common culprits include biotoxins, chronic infections, heavy metals, and industrial or household chemicals. Causative infections (discussed further here) include Cytomegalovirus, Human Herpesvirus 1 or 6, Lyme disease, dental bacteria that can travel to the brain (e.g. P. gingivalis) and various fungal infections (as mold toxins are notorious for causing cognitive impairment at all ages).
Type 3 uniquely causes widespread and often unpredictable neuronal death, occurs earlier in life—often between the forties and sixties—and is less strongly associated with genetic risk factors. Cognitive decline in this type is frequently accompanied by psychiatric symptoms, sensory changes, or executive dysfunction (e.g., difficulty with math, organization, executive tasks), rather than the more classic early Alzheimer’s memory loss.
Note: some of the most important neurotoxins to avoid are pharmaceuticals, and when I meet elderly individuals who have preserved their mental clarity, many report having largely avoided pharmaceuticals throughout their lives. Some of the most common problematic medications for brain health include certain high blood pressure medications (because they lower cerebral perfusion), statins (as they inhibit the production of compounds essential for brain function), acid reflux medications (which interfere with the absorption of vital brain nutrients—making it critical for everyone to have adequate stomach acid), antidepressants, antipsychotics, benzodiazepines, antihistamines (since, like many sleeping pills, they block restorative sleep), and anticholinergics (such as those prescribed for incontinence).
Type 4 — Vascular
In this form, chronic restriction of cerebral blood flow from existing vascular diseases leads to gradual neuronal injury and cognitive decline. Type 4 often appears in the seventies or beyond) and may overlap with other subtypes. It tends to affect processing speed, attention, and executive function rather than memory alone.
Note: rapid cognitive decline frequently followed COVID vaccination, and significantly overlapped with this type.
Type 5 — Traumatic
Severe head traumas or repeated concussions (e.g., in professional football players) sets off a cascade of chronic degenerative process which cause cognitive and emotional dysfunctional to appear years or decades after the injuries—making it critical to prevent these injuries and seek appropriate treatment when they happen.
Note: there are a variety of causes of dementia, many of which are frequently (roughly half the time1,2) misdiagnosed as Alzheimer’s. In many cases, these respond to the same treatments which reverse Alzhemer’s, but in other cases, require different treatments.
Healthy Fluid Circulation
Many practitioners I know who’ve successfully treating dementia with a variety of methods (listed here) all concluded it resulted from impairments of blood flow to the brain and lymphatic or venous drainage from it. For example:
•Zeta potential provides the disperse force which keeps constituents within fluids from agglomerating and clogging the circulatory vessels (e.g., vaccine frequently trigger detectable microstrokes by causing blood cells to clump together). In a myriad of illnesses, we find restoring the physiologic zeta potential (discussed here) is pivotal for restoring health—particularly those associated with aging, as zeta potential worsens with age (due to declining kidney function). In turn, one of the physicians who inspired my medical path did so because his practice revolved around treating zeta potential and he repeatedly achieved significant cognitive improvements for his aging patients.
Note: impaired zeta potential will also cause proteins (e.g., amyloids) to misfold and clump together.
•China recently developed a surgery (detailed here) to increase the lymphatic drainage from the brain. Due to its efficacy and low cost, it is being rapidly adopted around the country. In parallel, an American procedure was developed to increase venous drainage from the head and reported to greatly improve multiple sclerosis along with other chronic neuroimmune disorders (which distant colleagues witnessed).
Note: I have seen many other circulatory enhancing therapies (listed here) also improve cognitive decline and dementia.
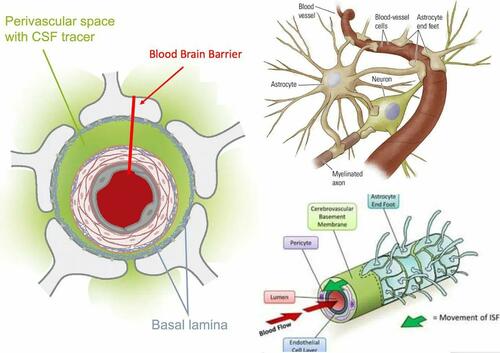
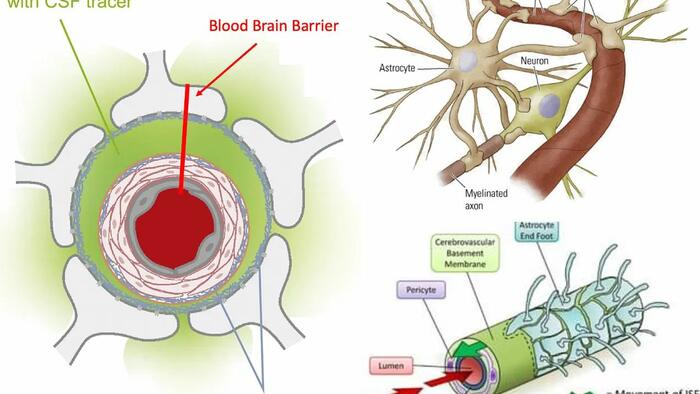
Furthermore, beyond blood being vital for neuronal survival, the proper clearance of waste products from the brain is as well. Unfortunately, due to how limited space is for the brain within the skull, robust lymphatic vessels do not exist, and instead, lymphatic drainage is created by astrocytes creating temporary lymphatic vessels around blood vessels during deep sleep.
This system, in turn, is highly vulnerable to disruption and numerous studies have now linked impaired glymphatic drainage to dementia (e.g., TBIs impair glymphatic drainage and adequate glymphatic drainage is required to eliminate amyloid from the brain)—which likely inspired the Chinese surgical procedure for dementia.
Due to the fragility of this system, things which disrupt it are quite consequential (e.g., poor zeta potential thickens and slows the drainage of glymphatic fluids). For example,